Prof. JULIE MILLER BA, MD, FRACS Specialist Endocrine Surgeon
What is the thyroid?
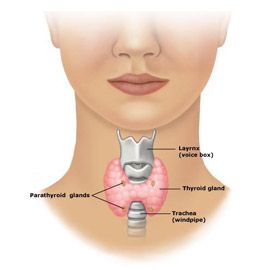
The thyroid is a butterfly-shaped gland that sits in your neck, draped across the windpipe and just under the larynx (voice box, adam's apple). It makes thyroid hormone, which controls your body's metabolism, including weight, heart rate, temperature, and mental alertness. An enlarged thyroid is called a "goiter." Most thyroids with a goiter or a lump still work properly, but some may be underactive or overactive.
Indications for thyroid surgery
There are several reasons to have thyroid surgery, including:
- To treat thyroid cancer that has been diagnosed by FNA (needle biopsy).
- To diagnose whether a lump is thyroid cancer when FNA (needle biopsy) is suspicious or inconclusive (AUS, follicular or Hurthle cell lesion, or neoplasm). Seventy-five percent (75%) of these turn out to be benign and require no further treatment. About 25% of these to prove to be cancer. If there is cancer, a second operation may be required to remove the rest of the thyroid gland.
- For pressure symptoms, coughing, difficulty swallowing or a choking feeling.
- If the nodule or gland is growing over time.
- If your doctor is concerned for other reasons like size, appearance, family history, or extension into the chest.
- For cosmetic reasons, if a large goiter is unsightly.
- As one of several options to treat an overactive thyroid.
Frequently Asked Questions
What are the potential complications of thyroid surgery?
The nerves that control your voice are closely associated with the thyroid gland. Temporary voice changes are common, but usually resolve within weeks to months. In ~1 in 100 parathyroid operations, the nerve that controls the voice is permanently injured, leaving your voice hoarse. Some patients have difficulty with projection of the voice and production of high pitched sounds. This problem is more common, and may affect your singing voice. “Voice fatigue” may occur as well, and is very common in the first few weeks.
Sometimes the parathyroid glands will not function well after a total thyroidectomy. These are four tiny, delicate glands that are located on the thyroid capsule. The parathyroid glands control calcium levels. If they don’t work, you will have low blood calcium. Therefore, some patients require calcium tablets on a temporary basis. If the parathyroids do not recover, calcium and vitamin D may be needed on a permanent basis. This occurs in about 2-3 in 100 total thyroidectomy operations.
There is a small risk of bleeding into the space where the thyroid used to be. If this happens, it may be necessary to have a second operation to evacuate the blood so it does not interfere with your breathing. Infection is relatively uncommon after this operation, but is easy to treat should it occur.
What are the risks of thyroid surgery?
As with anything in life, there are risks to surgery. These risks are weighed against the risks of not having surgery. Listed below are some of the possible complications of surgery. Risks include, but are not limited to:
- Permanent voice damage - 1%
- Permanent parathyroid damage(need calcium tablets) - 3% (total thyroidectomy only)
- Infection of Incision - Less than 1%
- Haematoma or Bleeding - Less than 1%
- Seroma (fluid collection, swelling) - 5% (higher for very large thyroids)
- Swelling and black/blue - About 5-10% (temporary)
- Needing thyroid tablets after removing half of thyroid - 20%
- Keloid or overgrown scar - uncommon in Caucasians, 10-20% in Asians, Indians, Africans
- Scar tethering/tightness - 5% early, usually settles with time
- Other unforeseen risks
You will require general an anaesthetic, given by a specialist anesthetist. I work with a select group of outstanding anaesthetists. Risk of a serious complication in a healthy person is very rare. Potential risks include, but are not limited to:
- Heart problems (death, heart attack, arrhythmias).
- Lung problems (pneumonia, wheezing).
- Blood clots (stroke, clots in leg veins or lungs).
- Drug reactions (also possible with local anaesthetic).
- Chipped teeth.
- Other unforeseen risks.
You will meet the anaesthetist before your operation and have the chance to ask any additional questions.
How much of my thyroid will be removed?
That depends on your condition. When the entire thyroid is removed, the operation is called a total thyroidectomy. You will need thyroid hormone replacement for life. A thyroid lobectomy or hemithyroidectomy is when half the thyroid is removed. In most instances (~80%), the remaining half can make enough thyroid hormone and you will not need tablets.
What type of anesthesia will I have?
You will have a general anesthesia. You will be completely asleep during the operation. You will have local anasthesia injected into the neck (cervical plexus block) to make you even more comfortable when you wake up. This local anaesthetic block will probably leave your ear lobes numb for 24 hours as well.
Will I have a scar?
Yes. All surgery causes a scar, and how a patient scars is dependent on the individual. A thyroid scar is a horizontal scar on the neck. The length of the scar depends on the size of your thyroid and the size of your neck, but is usually 5-6 cm (2-2.5 inches.) Techniques I use to minimize scarring include careful incision placement and hypoallergenic suture material (to avoid inflammation) I place my thyroid incisions in a natural skin crease, tailored to your individual neck and reason for surgery. Your scar may be higher than most other surgeons’ scars - in some patients the cosmetic result is better when the scar is in the shadow of the chin. In patients prone to keloids, I use skin glue rather than sutures. As a general rule, it is unusual to have a very noticeable scar after six months. Scars continue to fade for three years.
Will I have pain after the operation?
Most patients are surprised at how comfortable they are after thyroid surgery. Although you should be able to eat and drink normally, the main complaint is sore throat and discomfort with swallowing. Most patients take Panadol and/or Nurofen to keep them comfortable at home. You can have a prescription for something stronger for the first few days in case you need it, but beware prescription pain medicine can make you drowsy and constipated, so do not drive or operate heavy machinery, and drink lots of water and eat plenty of fruits and vegetables.
How long will I be hospitalized?
Most patients are admitted to the hospital on the morning of their surgery. If only half of your thyroid is removed, you may be able to go home that same evening, depending on how you feel. If you don’t feel well enough to go home, if your surgery was late in the day, if you live alone or far away, or if you’ve had the entire thyroid removed, you will be able to go home the next day.
When will I know the findings of the surgery?
A final pathology report requires careful study of the surgical specimen. Therefore, the final report is usually not available until about one week after the operation.
Will I have stitches?
You will have stitches on the inside that dissolve on their own. You will have a waterproof Comfeel dressing so that you can shower or bathe as usual (but do not submerge the incision for 5 days). Leave the dressing in place until your first post-operative visit, where it will be removed. If you have skin glue, it will eventually flake off by itself.
Will I have any physical restrictions after my surgery?
In general, your activity level depends on the amount of discomfort you experience. Many patients have returned to work and resumed most activities within a week or two after the operation, and you are able to drive as soon as you can turn your head comfortably without prescription pain pills (this limitation is for driver safety).
PREPARATION for SURGERY
Medications and Fasting
- Please shower at home the evening before or the morning of surgery
- For morning surgery, Do Not Eat anything after midnight the night before surgery unless otherwise instructed. You may drink clear liquids until one hour before your admission time. Clear liquids include black coffee, tea, water, clear broth or apple juice. No milk or other cloudy liquids. Medication with a small sip of water is OK. Your surgery may be cancelled if you do not follow these instructions.
- For afternoon surgery, a light breakfast BEFORE 7AM is OK, and clear liquids only after that, until one hour before your admission time. Clear liquids include black coffee, tea, water, clear broth or apple juice. No milk or other cloudy liquids. Your surgery may be cancelled if you do not follow these instructions.
- Do Not Drink Alcoholic beverages 24 hours prior to your surgery.
- Do Not Smoke for 4 weeks before surgery or your risk of serious complications increases.
- Please take heart, blood pressure, cholesterol, and reflux medicines as directed with a sip of water. For insulin or diabetic medications, please check with your anaesthestist.
- Diabetic SGLT2i medications MUST be stopped for 48 hours. This includes anything ending in “FLOZIN” (empagliflozin, ertugliflozin, canagliflozin, dapagliflozin) and brand names Invokana, Farxiga, Xigduo, Qtern, Jardiance, Synjardy, Steglatro, Segluromet, Stegluhan, and Glyxambi.
- Blood thinners: Stop aspirin or warfarin 5-7 days prior to surgery. Cease rivaroxaban (Xarelto) at least 24 hours before. Cease apixaban (Eliquis) at least 48 hours before. Discuss with your prescribing doctor if you need bridging injectable blood thinners.
- Do Not bring valuables such as money, jewelry etc. Do not wear make-up.
- Bring toiletries and loose fitting, comfortable clothing to wear upon discharge.
- You will be required to remove contact lenses, jewelry, dentures, and wigs.
- Arrange for a responsible adult to drive you home after discharge.
- Notify us if there is a change in your condition prior to surgery (such as a cold, cough, fever or infection). If severe, your surgery may need to be postponed for your safety.
- Stop all herbal medications 4 weeks before surgery unless discussed beforehand. Especially Fish oil, Ginseng, Garlic, and Gingko, St. John’s Wort, or Tumeric, which increase the risk of bleeding.
THE DAY of YOUR SURGERY
- On the day of your surgery, report to hospital reception at the appointed time.
- If you have not already done so, you will meet your anaesthetist.
- You may need a blood test or ECG prior to surgery.
- After the operation, you spend will some time in the recovery room before going to the ward.
- On the day of discharge, you are not permitted to:
- Drive a Car nor operate power equipment.
- Drink Alcoholic Beverages.
- Sign important papers.
The above are not permitted on the day of surgery, nor while taking any prescription pain medication. Instructions regarding safe resumption of the above activities will be provided by your surgeon.
Post-Operative Instructions for Thyroid or Parathyroid Surgery
Questions: call the office on .
Below are general instructions for patients who have had thyroid or parathyroid surgery. Since individual circumstances may vary, it is important that you discuss your individual post operative care with us.
Monitoring Your Progress
You should feel improvement every day after surgery. If you have any questions regarding your progress, call my office. You should make a follow up appointment approximately 1-2 weeks after your surgery.
Incision Care
Your incision is covered with a waterproof protective dressing. You can shower and wash your hair as usual, but do not soak or scrub the dressing. After showering, pat dry. Your dressing will be removed at your first post-operative visit. If you experience itching once the dressing is off, you may apply lotion to the scar. I recommend keeping Micropore tape on the scar (available at any pharmacy – it comes in brown or white – I think the brown looks better) for about 6 weeks. It will help the scar fade more quickly. Change it when it comes off on its own. Keep your neck and the scar moving by turning your head from side to side, tilting your head, and massaging your scar several times per day (with the tape in place).
You might notice bruising around your incision or upper chest and slight swelling behind the scar when you are upright. In addition, the scar may become pink and hard. This hardening will peak at about 3 weeks and may result in some tightness or difficulty swallowing, which will disappear over the next 3 to 4 months. You will also notice some numbness of the skin of your neck. This will gradually improve over time. Occasionally, patients get tethering of the scar on the inside, resulting in a tight feeling when swallowing or tilting the head back. If you experience this tightness, continue to stretch your neck and massage your scar firmly, several times per day. Turn your head back and forth and roll your shoulders. The tightness should settle down over time, usually by 3 months, but it continues to improve for three years.
Pain
The main complaint following parathyroid surgery is discomfort with swallowing. Some people experience a dull ache, while others feel a sharp pain. This should not keep you from eating anything you want, but the pain can be annoying for a day or two. Nurofen and/ or Panadol is generally enough to control this pain. Some people prefer Panadeine, but in general, stronger medications are not necessary for long. You may feel like you have phlegm in your throat. This is usually because there was a tube in your windpipe while you were asleep that caused irritation that you perceive as phlegm. You will notice that if you cough, very little phlegm will come up. This should clear up in 4 to 5 days. In a small proportion of patients, the “lump in throat” feeling persists for a few months, but in most cases is will eventually resolve.
Thyroid Hormone Tablets
If your whole thyroid was removed, you will be prescribed thyroid hormone tablets following surgery. You should take these on an empty stomach with water. Milk, food, and other pills interfere with your stomach’s ability to absorb the thyroid hormone. Six weeks after the operation, you will have a blood test to measure your levels of thyroid hormone and your dose of medication may be adjusted accordingly. Your thyroid hormone levels will then be measured about every 2 months until your hormone levels are stable (levels generally stabilize within 4 to 5 months).
Voice Changes
Your voice may go through some temporary changes with fluctuations in volume and clarity (hoarseness). Temporary changes are quite common. Generally, it will be better in the mornings and "tire" toward the end of the day. This can last for variable periods of time, but should clear in 4-6 months at most. There is a small (1/100) risk of permanent hoarseness. There is a higher chance your singing voice will be affected.
Hypocalcaemia after total thyroidectomy – tingling and numbness of fingers and toes
In many patients who have a total thyroidectomy, the parathyroid glands do not function properly immediately after total thyroidectomy. This is usually temporary and causes the blood calcium level to drop below normal (hypocalcaemia). Symptoms of hypocalcaemia include numbness and tingling in your hands, soles of your feet and around your lips, and can become quite unpleasant. Some patients experience a "crawling" sensation in the skin, muscle cramps or headaches. These symptoms appear between 24 and 48 hours after surgery. It is rare for them to appear after 72 hours. Low blood calcium does not occur if only half the thyroid is removed.
Hypocalcaemia is treated with calcium tablets. If you are having a total thyroidectomy, I will check a blood test before you leave, and send you home with calcium (big white pills) and calcitriol (little orange/red pills). If you develop pins and needles in your hands, feet, or lips htat lasts longer than 15 minutes, take two extra calcium tablets (there is no danger in taking it, even if you do not need it) The symptoms of tingling/numbness should improve within 30-45 minutes of taking the tablets. If the symptoms persist, you should take two more tablets and wait another 45 minutes. If they still persist after 3 extra doses, call my office in hours, or after hours report to your nearest emergency room to have your blood calcium checked.
Please keep us informed, and keep a record of the amount required. The hypocalcaemia usually disappears over a few weeks to months. In some cases (about 2% of all total thyroid operations), the parathyroid glands do not recover. If that happens, you will need to continue taking calcium tablets permanently, but typically not as many tablets as you needed in the first few weeks.
Bone Health
Patients who are taking thyroid hormone tablets or who have a history of parathyroid disease should consider taking Caltrate daily to promote healthy bones. In addition, an exercise routine using weights is also recommended.
CONTACT MY OFFICE for any of the following symptoms:
- Fever >38.3 or chills.
- Increasing pain or redness around incision.
- Difficulty breathing.
- Tingling around the lips or fingertips not relieved by extra calcium tablets.
- Severe muscle cramps.
AN IMPORTANT WORD ABOUT THE COSTS OF TREATMENT
Insurance rebates have not kept pace with the cost of running a medical practice. As a consequence, there will be a gap to pay for the surgical fee and for the anaesthetist. Your insurance company might also charge you an excess for a hospital admission. We will advise you about expected out-of pocket costs not covered by insurance. If these costs represent an undue hardship for you, please discuss them with us.
ASK YOUR DOCTOR
We are here to help you. If you have any questions, please ask. It is often helpful to bring a family member with you to a consultation, or to write questions down so you won't forget them.
